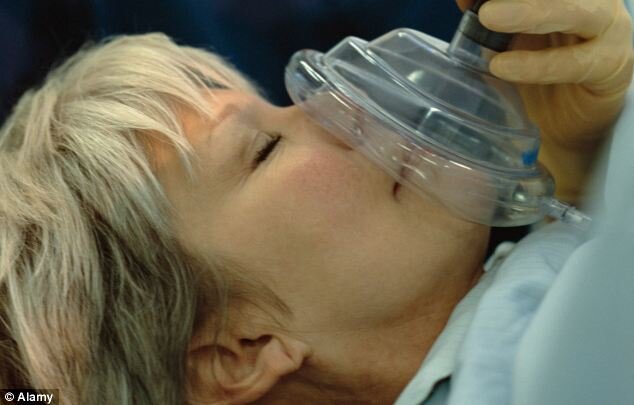
by Jenny Hope for Daily Mail:Having a general anaesthetic in later life could raise the risk of developing dementia by a third, warn researchers. Brain changes caused by the anaesthetic could lead to Alzheimer’s within a few years in some patients, according to a study.It has long been known that having a general anaesthetic may result in poor brain functioning straight after an operation, especially in the elderly. In most cases the side-effect is temporary, although many relatives complain their loved ones were ‘never quite the same’ after a major operation.There has already been debate over whether there is a link with dementia in the long term. Last year research on mice suggested cognitive function could be impaired in ways similar to changes caused by Alzheimer’s. The latest study found a 35 per cent higher risk of dementia in older people having surgery under general anaesthetic compared to local anaesthetic.
Extra cases of dementia emerged among patients up to eight years later, according to the study by the French Institute of Health and Medical Research and the University of Bordeaux.British experts said there was rarely an alternative to general anaesthetic if older patients need major surgery but more research could help identify those at risk.Researchers analysed medical data French people aged 65 and over living in three cities. They were interviewed at the start of the study and subsequently two, four, seven and ten years after.Each examination included a complete assessment of cognitive functioning and systematic screening for dementia.After two years, researchers started asking 7,008 participants whether they had undergone a general or local anaesthetic since the last follow-up. The data was adjusted to take account of factors such as socioeconomic status and other medical conditions which might raise the risk of dementia.Altogether 19 per cent had undergone a general anaesthetic and 14 per cent has been treated under a local anaesthetic. A total of 632 people – nine per cent – developed dementia over the eight subsequent years of the study, most of whom were diagnosed with Alzheimer’s.The research was presented yesterday at Euroanaesthesia, the annual congress of the European Society of Anaesthesiology in Barcelona.The researchers said the change in the brain that causes cognitive dysfunction after major surgery is the same as the one that causes dementia – when clumps of a protein stick to brain cells, affecting memory, mood and behaviour.Several studies have suggested that some anaesthetic drugs could promote inflammation of brain tissue in a way that is characteristic of dementia.Another theory is that insufficient oxygen to the brain may have an effect in vulnerable patients.Dr Eric Karran, of charity Alzheimer’s Research UK, said: ‘We need to await the full peer-reviewed publication before fully interpreting the results.‘Research into the impact of anaesthetics on dementia is challenging. Dementia is caused by several brain diseases, many of which arise from a complex mix of genetic and environment factors.‘Understanding these risk factors is vital, but research into dementia remains poorly funded compared to other diseases. We need to see sustained funding to unravel the full complexity of this devastating condition.’Source:
http://dailym.ai/12nf5QEPicture: Alamy